Sustainability has yet to make an impact in terms of materials and circularity.
Textiles are widely used in medical, surgical and other healthcare applications, including first aid and clinical settings, ranging from surgical gowns and drapes, compression garments and fracture management products, to more sophisticated items, such as advanced wound dressings, surgical sutures, vascular grafts and tissue scaffolds.
Surgical textiles
Textiles used in surgical and healthcare environments include surgical gowns and other apparel, drapes, sterilization wraps, face masks, staff uniforms, hospital bedding, mattress covers, curtains and medical wipes. These products are used in hospital operating rooms, emergency rooms, clinics and doctors’ offices, both to protect healthcare personnel and to maintain a sterile environment.
Surgical textiles in particular must be non-toxic, biocompatible and comfortable, with the fabrics having properties of durability, strength and elasticity, as well as the ability to prevent infection and contamination.
At present, most textiles used in surgical settings are single-use (disposable) with multi-use (reusable) products accounting for less than half – and possibly as low as 30% – of the global market.
Although manufacturers of single-use products face strong competition from reusable textiles, there is a growing usage and acceptance of disposable medical products worldwide.

The use of disposable products is highest in the U.S. and Europe, while in most other major markets, with the exception of Japan and Australia, reusable textiles are predominantly used.
Demand for surgical textiles is growing as a result of increasing demand for safety and economy. Another driver is the rising number of hospital stays, which is particularly the result of the increased age structure of the population in developed countries.
Protection of medical personnel
The protection of medical personnel, particularly in surgical settings, from viral exposure has never been more important, especially during the COVID-19 pandemic.
In recent decades, the world has also witnessed an increasing incidence of other viruses and contagious diseases, such as human immunodeficiency virus (HIV), methicillin-resistant Staphylococcus aureus (MRSA), Creutzfeldt-Jakob disease (CJD), hepatitis and severe acute respiratory syndrome (SARS), as well as persistent outbreaks of avian and swine influenza.
The global rise in the prevalence of nosocomial infections, otherwise known as hospital-acquired infections (HAIs), has also added to the cyclical parade of pathogens in hospitals and healthcare facilities.
Advanced wound care
A key area of the medical textiles industry is advanced wound care, with the global market estimated to be worth US$9 billion in 2018 and expected to reach US$13.3 billion in 2025, with a compound annual growth rate of 5.85% from 2019 to 2025, according to a recent report from Brandessence Market Research & Consulting.
The market is expected to witness significant growth owing to rising awareness about the benefits of advanced wound care together with technological advancements. In particular, an increasing number of new products are enhancing growth, while innovations to improve product functionality are creating new market opportunities.
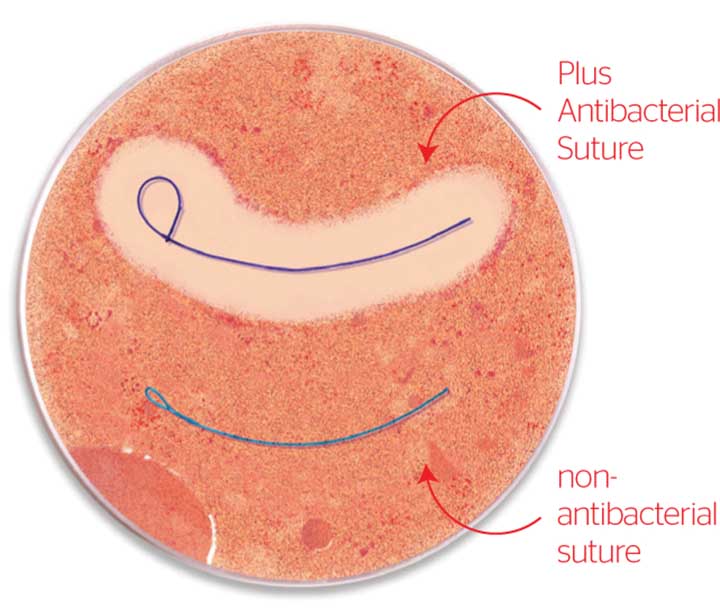
Advanced wound care products play a pivotal role in treating chronic or acute wounds, which are particularly associated with conditions such as diabetes mellitus, weak immune systems, cardiovascular or respiratory disease, renal impairment, malignancy, rheumatism, obesity and malnutrition.
Moreover, both the growing geriatric population, which is at high risk of developing chronic wounds, and increasing healthcare expenditure in most countries are fostering market growth.
Advanced wound care remains a major issue for public health budgets and the global economy in general. The report estimates that 2% of all patients worldwide require chronic wound care, with a growing incidence in the increasing elderly population, particularly diabetic foot ulcers.
Further, among all chronic wounds, 70% recur and 34% exhibit infection. Increased penetration of chronic diseases such as diabetes, the association of chronic wounds with morbidity and a rapid increase in the aging population are primary concerns for global healthcare systems.
Fiber classification
A wide range of natural and man-made fibers are used to manufacture medical textiles, depending on the characteristics required for the end product.
Synthetic polymers, which are used extensively, may be permanent, such as polyamide, polyester, polyethylene, polypropylene, polytetrafluoroethylene, polyurethane and polyacrylonitrile, or biodegradable, such as those used in sutures and tissue engineering structures, such as polycaprolactone, polyglycolic acid and polylactic acid.
Besides cotton, silk and regenerated cellulose such as viscose and lyocell, natural fibers used in medical textiles include biodegradable polymer fibers made from, for instance, chitin, collagen and alginate.
Efficacy and durability are key performance features of most medical textiles, although biodegradable fibers can be employed in certain implantable devices, such as surgical sutures, vascular and cardiovascular grafts and tissue scaffolds, where degradation over a specific time period is a requirement.

Disposal
However, while performance and safety are key properties of medical textiles, the issue of sustainability has yet to make much of an impact in terms of the fibers used and the recyclability of the end product.
The COVID-19 pandemic and the huge increase in the production and use of face masks, as well as disposable test kits, which has created more waste and problems with littering, has highlighted the ongoing issue of single-use plastics and their safe disposal.
Products such as wound dressings are frequently made of laminates or composites, which makes their recycling virtually impossible, let alone the issue of possible contamination with pathogens. Incineration of hospital textile waste seems to be the most likely option for the foreseeable future, at least from a safety point of view.
Similarly, apart from the existing utilization of natural fibers, such as cotton, and regenerated cellulose fibers in certain applications, the use of more sustainable and/or biodegradable fibers has yet to make much of an impact on the medical textile industry. Further developments in synthetic fibers appear to be key for the near future in this market.
Tissue engineering
Despite such an environmentally pessimistic outlook, natural materials have been gaining popularity in recent years as sustainable alternatives for use in tissue engineering. For example, U.S. researchers from the University of Florida have developed methods of growing cells and tissues using a biocompatible textile mesh made from a woven natural fiber mat from the Manicaria saccifera palm.
Meanwhile, scaffolds made with electrospun fibers comprising a bioactive peptide component of a soy protein isolate have recently been constructed for wound healing and tissue regeneration applications by scientists at Temple University in Philadelphia, Pennsylvania, USA.
Sustainable wound care
At November’s Compamed medical technology trade fair in Düsseldorf, Germany, Freudenberg Performance Materials highlighted its multi-layer material compositions of foams and nonwovens for what it calls “sustainable wound care.”
The company’s Eco-Check label endorses particularly sustainable solutions for the design of wound plasters that use bio-based raw materials, allowing biodegradation in an industrial composting setting after the product has been used.
M 1701 for traditional wound care plasters comprises 100% polylactic acid derived from natural resources and is said to offer good wound care characteristics, while M 1714 has superior absorption for more challenging wounds and consists of a mix of bio-based fibers.
With a smooth wound contact layer, M 1714 has already been evaluated for industrial compostability and conforms to ISO 13432, said the Weinheim, Germany-based company.
In addition, Freudenberg’s silicone-coated foams have several improved features that reduce the number of process steps in wound dressing manufacturing to decrease production complexity, avoiding waste, saving energy and simplifying the supply chain.
The solution is said to maintain all the advantages of a pure foam dressing without a silicone layer, such as free swelling and prevention of exudate pooling in the wound bed, while eliminating the disadvantages of solutions with standard silicone adhesive layers.
From a nursing perspective, advantages include higher flexibility that enables optimal wound bed contouring and the reduced risk of infection owing to the prevention of exudate pooling.

Spider silk technology
Meanwhile, biotechnology company Kraig Biocraft Laboratories has announced the first sample shipment of its recombinant spider silk fibers and fabrics for use and evaluation into a range of biomedical applications.
The shipment was made from its production operations in Vietnam in response to a recent increase in requests for its proprietary spider silk technology for tissue engineering applications, said the company of Ann Arbor, Michigan, USA.
Aided by its unique blend of mechanical and chemical properties, spider silk has long been recognized as an ideal, natural biomaterial. As a lightweight, biocompatible and biodegradable material, spider silk applications have been tested in numerous products, including fibers, films, hydrogels, nonwovens and foams.
While the first known cases of sutures made from spider silk date back to the 18th century, limitations in the production and costs of spider silk have so far prevented its broad adoption.
Kraig Labs’ approach of recombinant spider silk technology utilizes genetically enhanced silkworms, which could enable the large-scale adoption of spider silk for biomedical applications.