The Georgia Tech Pressure Injury Prevention System.
Our vision is to “make pressure injury a scourge from the past.” A pressure injury (PI) is localized damage to the skin and underlying soft tissue usually over a bony prominence or related to a medical or other device[1]. The injury results from intense and/or prolonged pressure or pressure in combination with shear, and coupled with moisture. Individuals with spinal cord injuries (SCI) are at a higher risk for PI because of reduced sensory perception, which makes PI a serious, lifelong complication with the potential to “interfere with physical, psychological and social well-being and to impact overall quality of life”[2]. While preventable in most situations, when PI occurs, they may “disrupt rehabilitation, prevent individuals with SCI from attending work or school, and interfere with community reintegration”[3]. Thus, there is a critical need for a cost-effective intervention that will address a significant issue affecting the quality of care (and hence quality of life) for individuals with SCI, and, in the process, reduce healthcare costs, which, in 2020, accounted for 19.7% of GDP in our nation[4].
Our mission has been to design and develop an end-to-end system comprising a fabric-based sensor network, signal-processing hardware, knowledge-processing software, an actuator-based intervention hardware, and a smartphone App to prevent the occurrence of PI.
The existing solutions
A common practice to relieve the constant pressure at the contact points between the individual and the seating surface is to reposition the individual every two hours. The time interval of two hours is a rule of thumb practiced in hospitals. While it is possible for the nursing staff in a hospital to reposition the individual every two hours, it is not easy for individuals with SCI to reposition themselves; they would need the help of a caregiver. COVID-19 exacerbated the shortage of caregivers, which left many of the individuals without this critical support. Wedges, cushions, specially designed seats, and air pads are a few of the devices used to mitigate pressure injury. While helpful, they are passive devices and do not respond dynamically depending on the specific individual or situation. Furthermore, their functionality falls into either the “offloading” mechanism or the “immersion” mechanism for relieving the pressure at the contact point.
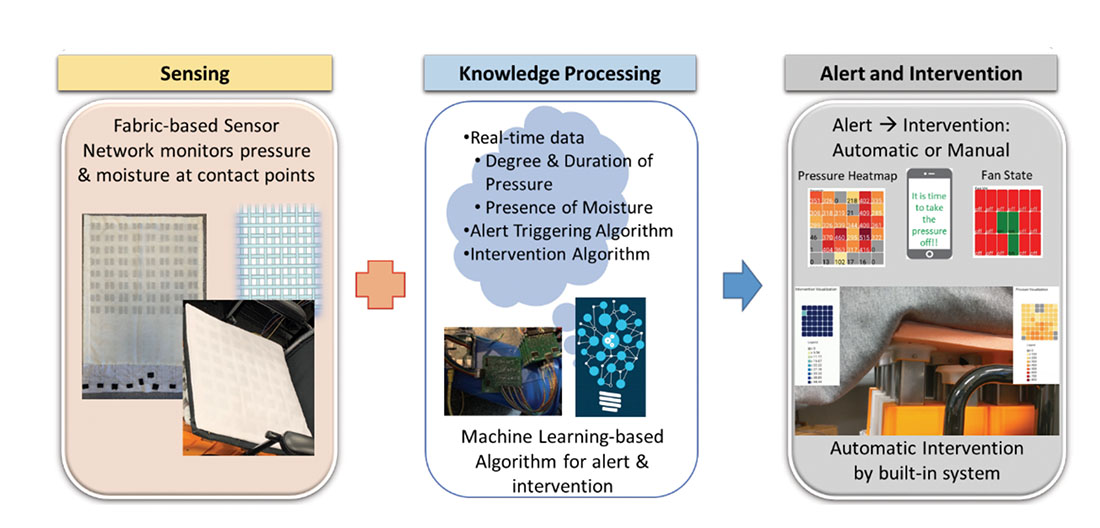
Our solution – the Georgia Tech Pressure Injury Prevention System – continuously and unobtrusively monitors pressure and moisture at an individual’s contact points with a surface (e.g., bed, wheelchair) and applies machine learning to harness the acquired data to trigger an evidence-based alert and provide a knowledge-based intervention in real-time to relieve the pressure and moisture in the specific body part and thereby prevents a PI. Figure 1 shows the conceptual framework for the system integrated into a wheelchair at Georgia Tech along with the technology building blocks.
As shown in Figure 1, the Sensing Technology building block consists of a fabric-based sensor network, which continuously monitors the pressure and moisture at the surface contact points of the individual seated in the wheelchair. The Knowledge Technology building block is responsible for processing the pressure and moisture signals from the Sensing Technology building block, and determining the need for intervention to prevent the occurrence of a PI. When a specific threshold is reached for one or both the parameters (pressure and moisture), which indicates the potential for a PI, the appropriate alert is triggered. The alert is handled in one of two ways: manual or automatic. In the automatic mode, the Intervention Technology building block triggers the intervention based on the data and rules in the system; in the manual mode, the system recommends the specific intervention (again based on data and rules) and the individual with SCI has the option to accept or reject the recommendation to trigger the intervention on the App. The App provides a real-time heatmap of the pressure and moisture levels at the surface contact points. It also displays the position and status of the actuator system and the fan system, respectively.

Figure 2 shows the Georgia Tech Pressure Injury Prevention System integrated into a wheelchair. The fabric-based sensor network is placed on the seat. The underside of the wheelchairs shows fans, which are triggered by the intervention system to reduce the moisture leveled at the surface contact points. The end-to-end system has been tested successfully in the lab.
Platform for big data analytics
The Georgia Tech Pressure Injury Prevention System provides an easy-to-use platform for acquiring data unobtrusively from individuals with SCI in wheelchairs, both in real-time and over long duration. This treasure trove of data can be analyzed and mined to determine personalized interventions to prevent PI. In the long-term, the data will serve as the foundation for understanding the needs of individuals in wheelchairs and used to enhance the design of wheelchairs and other aids to prevent PI, especially for those with SCI.
While the focus of the discussion has been on preventing PI in individuals with SCI, our solution is not restricted only to them – it is applicable to all situations when an individual is in contact with a surface for extended periods. For example, individuals confined to beds for long periods in hospitals and in nursing homes are susceptible to PI as are drivers in long-haul transportation and individuals seated in office chairs for long durations. This is due to the fact that a fabric is the ideal platform that can serve as an effective information infrastructure for the distributed network of sensors because textile fabrics are shape-conformable, breathable, drape well, soft, and comfortable[5]. Thus, the Georgia Tech Pressure Injury Prevention System will make a significant contribution to enhancing the quality of life for individuals by preventing the occurrence of pressure injuries and pave the way for making “pressure injury a scourge from the past.”
Acknowledgements: The authors gratefully acknowledge funding for the research from the Imlay Innovation Fund and the Craig H. Neilsen Foundation under a Pilot grant in the Spinal Cord Injury Research on the Translational Spectrum program. They also thank the following members of their research team for their various contributions: Nikhil Soraba, Aditya Chavan, Shiv Chopra, Kyle Motter, Xandy Liu, and Chengjia Shao.
References
- National Pressure Ulcer Advisory Panel, 2016, Washington, D.C.
- Consortium for Spinal Cord Medicine. Pressure ulcer prevention and treatment following spinal cord injury: A clinical practice guideline for health care professionals, 2000.
- Houghton PE, Campbell KE and CPG Panel (2013). Canadian Best Practice Guidelines for the Prevention and Management of Pressure, Ulcers in People with Spinal Cord Injury: A resource handbook for Clinicians.
- National Health Expenditures Highlights, https://www.cms.gov/Research-Statistics-Data-and-Systems/Statistics-Trends-and-Reports/National HealthExpendData/NationalHealthAccounts Historical, 2021.
- Park, S., and Jayaraman, S., “Wearable Sensor Networks: A Framework for Harnessing Ambient Intelligence,” Journal of Ambient Intelligence and Smart Environments, Vol. 1, No. 2, 117-128, 2009.